Organ Trafficking and Transplant Tourism: A Commentary on the Global Realities
Abstract
The extent of organ sales from commercial living donors (CLDs) or vendors has now become evident. At the Second Global Consultation on Human Transplantation of the World Health Organization’s (WHO) in March 2007, it was estimated that organ trafficking accounts for 5–10% of the kidney transplants performed annually throughout the world. Patients with sufficient resources in need of organs may travel from one country to another to purchase a kidney (or liver) mainly from a poor person. Transplant centers in ‘destination’ countries have been well known to encourage the sale of organs to ‘tourist’ recipients from the ‘client’ countries.
Organ trafficking brings little regard for the well being of the donor. Who cares for the donor in the early period following transplantation or in the long term, especially if complications arise? This report will describe the organ trafficking known to the authors by their visits to many countries on behalf of The Transplantation Society (TTS) and the World Health Organization and by the field research and advocacy work with commercial living donors (CLDs) of the Coalition for Organ‐Failure Solutions (COFS). It introduces alternative approaches that must be addressed by each country to combat organ trafficking.
The buying and selling of organs in the global markets has become an ethical issue for transplant clinicians everywhere in the world. Even physicians who would have no part in the organ trade now bear a responsibility for the medical care of those recipients who return to their home countries having undergone organ transplantation from an unknown vendor. These recipients arrive at physician offices in widespread locations such as Tel Aviv, Toronto and Trinidad. Some patients return home with inadequate reports of operative events and unknown risks of donor‐transmitted infection (such as hepatitis or tuberculosis) or a donor‐transmitted malignancy. The source of their allografts is mainly from the poor and vulnerable in the developing world. These vendors or commercial living donors resort to an organ sale because they have virtually no other means to provide support for themselves or their families. Selling kidneys may be a consideration of ‘autonomy’ in academic debate but it is not the coercive reality of experience when a kidney sale is a desperate alternative available to the poor (1).
This report describes the characteristics and extent of the global trafficking in human organs. It includes the experience of the authors’ personal visits to numerous countries on behalf of TTS and WHO. This report is also fashioned by the extensive field research of COFS. Finally, this commentary proposes an alternative approach that must be addressed by each country to alleviate the shortage of organs for transplantation and combat the exploitative practices of organ trafficking.
Definition of Organ Trafficking and Transplant Tourism
The discourse on the market of organs has used various terms to describe the commercialism at the core of organ trafficking. The seller of a kidney is not only the donor source of an organ but a vendor whose motivation is monetary gain. The following definition of organ trafficking is derived from the United Nations Trafficking in Persons (2). Organ trafficking entails the recruitment, transport, transfer, harboring or receipt of persons, by means of the threat or use of force or other forms of coercion, of abduction, of fraud, of deception, of the abuse of power, of a position of vulnerability, of the giving or receiving of payments or benefits to achieve the consent of a person having control over another person, for the purpose of exploitation by the removal of organs, tissues or cells for transplantation. The reason to oppose organ trafficking is the global injustice of using a vulnerable segment of a country or population as a source of organs (vulnerable defined by social status, ethnicity, gender or age).
This definition of organ trafficking captures the various exploitative measures used in the processes of soliciting a donor in a commercial transplant. Exploitation is the threat or use of force or other forms of coercion, abduction, fraud, deception, abuse of power or position of vulnerability. The commercial transaction is a central aspect of organ trafficking; the organ becomes a commodity and financial considerations become the priority for the involved parties instead of the health and well‐being of the donors and recipients.
Transplant Tourism has become a connotation for organ trafficking. The United Network for Organ Sharing (UNOS), recently defined transplant tourism as ‘the purchase of a transplant organ abroad that includes access to an organ while bypassing laws, rules, or processes of any or all countries involved’ (3). However, not all medical tourism that entails the travel of transplant recipients or donors across national borders is organ trafficking. Transplant tourism may be legal and appropriate. Examples include, when travel of a related donor and recipient pair is from countries without transplant services to countries where organ transplantation is performed or if an individual travels across borders to donate or receive a transplant via a relative. Any official regulated bilateral or multi‐lateral organ sharing program is not considered transplant tourism if it is based on a reciprocated organ sharing programs among jurisdictions.
The modes of illicit transplant tourism were recently illustrated by Yosuke Shimazono at the Second Global Consultation on Human Transplantation at the WHO headquarters in Geneva in 2007 (Figure 1) and capture the various ways recipients, CLDs, and transplant centers may be coordinated for such a transplant (4). In addition to these modes that occur across national borders, organ trafficking may also occur at transplant centers within the same country of residence of the CLD and recipient.
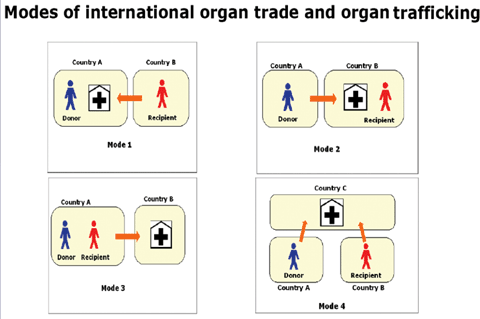
Figure 1
In this figure, Shimazono (2007) illustrates four modes of transplant tourism. Mode 1 entails a recipient traveling from Country B to Country A where the donor and transplant center are located, Mode 2 entails a donor from Country A traveling to Country B where the recipient and transplant center are located, Mode 3 entails a donor and recipient from Country A traveling to Country B where the transplant center is located, and Mode 4 entails a donor from Country A and a recipient from Country B traveling to Country C where the transplant center is located.
The Extent of Organ Trafficking
Countries that have facilitated organ trafficking such as Pakistan and the Philippines do not release precise data (not surprisingly) regarding the numbers of foreign patients that travel to these countries for transplants. In the Philippines, a quota of foreign nationals was intended but there has been no report of data to indicate that such a stipulation has been fulfilled. Despite its clandestine nature and the difficulties in obtaining national data, the extent of organ trafficking has become evident by our visits to many countries around the world and by reports prepared for presentation at the WHO.
According to data from the Sindh Institute of Urology and Transplantation (SIUT), at least 2000 kidney transplants have been performed in Pakistan to transplant tourists (source: Delmonico visit to Karachi Pakistan January 2007). The widespread dimension of these practices becomes particularly evident, when a highly regarded nephrologist in Port of Spain Trinidad reports that a series of 80 patients had gone from Trinidad to Pakistan to buy organs (source: Delmonico visit with Dr. Leslie Ann Roberts in Trinidad).
In the Philippines, a February 2007 newspaper account of the number of kidney sales reveals over 3000 have been performed (5). The WHO held a regional consultation in Manila to call attention to its objection to the rampant commercialism (source: Delmonico participation). The Cebu Province of the Philippines is now reported to be seeking transplant tourists to increase Philippine commercial transplants (6).
It is estimated by Egyptian transplant professionals that we both have visited (source: Egyptian Society of Nephrology, Cairo June 2007) that Egypt performs at least 500 kidney transplants annually (7). A majority of these transplants are performed from CLDs.
Scott Carney reports (source: conversations with Delmonico and by Carney publications) that transplant tourists have undergone kidney transplantation from tsunami victims in Chennai, India (8).
At the WHO regional consultation in Slovenia, the representative from Moldova reported the request of Israeli physicians to set up a transplantation practice in that country. The request was denied but there is no current penalty being imposed upon the insurance companies that are systematically enabling these transplants to occur outside of Israel. As many as 20 patients from Israel may currently undergo kidney transplantation in the Philippines each month. The consequence for Israel is that the expertise in performing organ transplantation within Israel may be lost (9). Hopefully, the pending legislation in the Knesset on organ transplantation will address this issue (see below).
At the Second Global Consultation on Human Transplantation at the WHO headquarters in Geneva in 2007, Shimazono also assembled a sampling of the trafficking by an analysis of databases such as Lexis/Nexis, MEDLINE and Pubmed academic journal articles, and Google searches that included media sources, transplant tourism websites, renal and transplant registries and reports from health authorities. Shimazono estimated that 5–10% of kidney transplants performed annually around the globe are currently via organ trade. The credibility of this estimate is given by the following data: at least 100 nationals from countries such as Saudi Arabia (700 in 2005), Taiwan (450 in 2005), Malaysia (131 in 2004) and South Korea (124 in the first 8 months of 2004) went abroad annually for a commercial kidney transplant. At least 20 nationals from other countries such as the Australia, Japan, Oman, Morocco, India, Canada and the United States traveled as transplant tourists for trafficked organs. But the more striking observation comes from the revelation of data in a visit to China in the summer of 2007. In 2006, 11 000 transplants were performed in China from executed prisoners. There were 8000 kidney transplants, 3000 liver transplants and approximately 200 hundred heart transplants. The 8000 kidney transplants alone in China in 2006 would account for at least 10% of the total number of annual organ transplants done in programs of organ trafficking. It should be noted that since China’s recently adopted Human Transplantation Act that bans commercialism was adopted in May 2007, China has reduced the number of transplants to foreign patients by 50% in 2007. Nevertheless, the reduction in Chinese activity has presumably been supplanted by an increase in Philippine organ trafficking.
Merion et al. have reported the initial US experience that includes some patients whose transplants were not obtained from CLDs (10). One hundred nineteen US citizens and resident aliens from 55 transplant centers in 26 states were recorded as having received kidney transplants in 18 foreign countries after a median of 1.5 years (range 21 days to 8.5 years) on the US waiting list. HRSA officials who collaborated with Dr. Merion are now aware of this practice and should be following it closely. There is a public hazard for patients to return from out of country was potential transmissible infection such as avian flu, tuberculosis, Schistosomiasis, acute hepatitis and/or HIV infection.
Recipients of commercial transplants abroad should not be denied the provision of follow‐up care; yet there is no justification to condone illegal transplants outside United States if the purchase of a kidney (that could result in Medicare benefits to be received for immunosuppressive medications) is illegal within the borders of the United States. The legislation that is being considered by the Knesset in Israel would prohibit the insurance reimbursement of transplant costs for Israelis that undergo a purchased organ transplant in countries where the buying and selling of organs is illegal.
Insurance companies may be influencing practices: for example, Bramstedt and Xu reveal ‘US medical insurance programs are taking steps to address the problems of organ availability, long waiting times, and high medical and surgical costs by promoting transplant tourism’ (11).
The Consequence to the Vendors
What then of this emerging worldwide population of live kidney vendors? In Pakistan, the SIUT group has carefully detailed a sample cohort of (n = 239) vendors in a follow‐up—the outcome all very troubling (12). The majority of these CLDs (93%) who sold a kidney to repay a debt and (85%) reported no economic improvement in their lives, as they were either still in debt or were unable to achieve their objective in selling the kidney. The disturbing report by the SIUT group becomes not only an accounting of the Pakistani experience but an indictment of the international transplant community because it overlooks the plight of the donor whose interests are just as valid as the recipients.
Egypt is one of the few countries that prohibits organ donation from deceased donors. In the absence of an entity to govern allocation or standards for transplants, the market has become the distribution mechanism. Egypt is also one of the countries in which COFS has conducted extensive field research and long‐term outreach service programs for victims of the organ trade. In‐depth longitudinal interviews conducted by Budiani reveal that 78% of the CLDs (n = 50) reported a deterioration in their health condition. This is likely a result of factors such as insufficient donor medical screening for a donation, pre‐existing compromised health conditions of CLD groups and that the majority of employed CLDs reported working in labor‐intensive jobs. A kidney sale does not solve the most frequently given reason for being a CLD, 81% spent the money within 5 months of the nephrectomy, mostly to pay off financial debts rather than investing in quality of life enhancements. CLDs are not eager to reveal their identity; 91% expressed social isolation about their donation and 85% were unwilling to be known publicly as an organ vendor. Ninety‐four percent regretted their donation (13).
The studies in Pakistan and Egypt are consistent with findings in India (14), Iran (15) and the Philippines (16) that revealed deterioration in the health condition of the CLDs. A long‐term financial disadvantage is evident following nephrectomy from a compromised ability to generate a prior income level. The common experience also entails a social rejection and regret about their commercial donation. These reports are consistent with the COFS experience in the CLD interviews; a cash payment does not solve the destitution of the vendor.
What Are the Alternatives?
As an international community we need to fulfill the goals of the Amsterdam Forum and provide ethical protocols for donor selection and longitudinal care for the live kidney donor (17). We collectively need to dispel the unrealistic notion that these cash payments can be regulated without the influence of brokers. The cash payment system targets the poor, privileges those who can afford the purchase, undermines altruistic donation and it has escaped governmental regulation. The Iranians are to be commended for their candor at a recent Transplantation Society Key Opinion Leader meeting in Turkey in which Professor Ahad Ghods and his colleague Dr. Shokoufeh Savaj acknowledged limitations of the Iranian Model, which included the lack of medical coverage for the donor beyond one year following transplantation. But it is also widely known that unregulated payments may be imposed upon the recipient.
Transplants conducted in countries with loose or no legal frameworks such as that of Pakistan, the Philippines and Egypt accommodate the organ market and the transplant tourists that drive the demand. Engaging governments to play a central role in establishing laws on transplants and for the Ministry of Health to carry out oversight of transplant practices is an essential component to improve the global situation of organ trafficking/transplant tourism. This has been the gratifying experience of TTS interaction with the Chinese Ministry of Health, but it remains to be determined if MOH regulatory oversight will be sustained after the 2008 Beijing Olympics. An alliance of TTS and the International Society of Nephrology (ISN) and other professional societies, all working with the WHO to influence health authorities at the World Health Assembly is now needed to combat organ trafficking.
Each country should establish a system of deceased organ donation. At a WHO Regional Consultation on Developing Organ Donation from deceased donors, held in Kuwait City last year, transplant professionals from Bahrain, Iran, Jordan, Kuwait, Lebanon, Libya, Morocco, Oman, Pakistan, Qatar, Saudi Arabia, Sudan, Syria, Tunisia, United Arab Emirates and Yemen supported the development and expansion of organ and tissue donation from deceased donors. They opposed commercialism and transplant tourism, including brokerage and medical professionals seeking monetary profit as a result of the vendor sale or coerced donation of an organ or tissue. The Kuwait Statement was crafted with an eye towards the following goals:
- Each country must develop a legal framework and national self‐sufficiency in organ donation and transplantation;
- Each country must have a transparency of transplantation practice that is accountable to the health authorities and whose authority is derived from national legislation;
- Countries in which the buying and selling of organs is outlawed must not permit their citizens to travel to destination countries and return for insured health care in the client country and
- Insurance companies should not support illegal practices as they are doing preferentially in some countries.
This list is not exhaustive of approaches that can improve the care of the live donor consistent with the recommendations of the Amsterdam Forum. Proposals are now being made to address additional measures to improve donor safety (18). These aims of the Kuwait Statement are also elaborated in the drafted and updated WHO Guiding Principles. This document is a product of the recommendations from global experts who participated in several WHO regional consultations hosted in diverse locations such as Khartoum, Manila, Slovenia and Geneva. The WHO guiding principles emphasize that ‘organs, tissues and cells should only be donated freely and without monetary reward. The sale of organs, tissues and cells for transplantation by living persons, or by the next of kin for deceased persons, should be banned. However, the prohibition of sale or purchase of cells, tissue and organs does not affect reimbursing for reasonable expenses incurred by the donor, including loss of income, or the payment of other expenses relating to the costs of recovering, processing, preserving and supplying human cells, tissues or organs for transplantation’.
Additionally, corporations such as pharmaceutical companies involved in transplants and insurance companies should also be made accountable for their engagement in processes, which prioritize profit generation at the disregard of social justice. TTS has addressed each of the major pharmaceutical representatives involved in transplantation (Delmonico Sydney Australia August 2007) to solicit support for its global mission to combat organ trafficking. Further, various insurance programs (both public and private) in countries as diverse in resources as the US, Israel, Yemen and Saudi Arabia, should not encourage patients to seek a transplant abroad without regard to the source of the organ (11, 19). These countries cannot overlook the plight of the donor and condemn organ sales within the country and condone the commercialism outside its borders. There is precedent in international law to prohibit illegal practices irrespective of national borders, for example, in the bribery of public officials (20).
The international transplant community must deliver a concerted message that organ markets that exploit the poor and vulnerable are not acceptable, but programs must be developed alternatively that assure donor safety and provide social benefits that address donor needs. These needs are the legitimate consequences of living organ donation and must be addressed in each country with Ministry of Health oversight, authorized by national legislation and guided by the World Health Assembly resolution.
